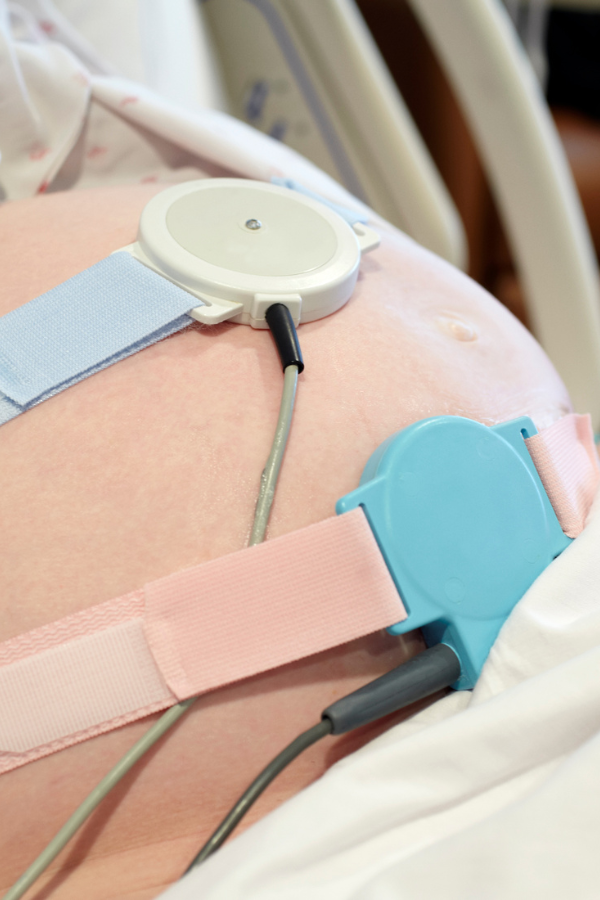
You have probably heard the term postpartum hemorrhage if you’ve done some learning about birth. And my guess is, if the convo stopped there, you may have ended up a little bit scared! Postpartum hemorrhage is an aspect of birth it’s important to know about. But it is a disservice when we simply tell you it’s a complication and we don’t teach you anything else. We are going to get into together, okay?
Who is The Labor Mama and Why Am I Here?
Hey friend! I’m Lo – also known around here and social media as The Labor Mama. I’ve spent my nursing career in labor, delivery, and postpartum, have birthed 4 of my own babies, have labored thousands of mamas at the bedside, have taught hundreds of students online, and have even delivered a few speedy little babies with my bare hands (oops).
Here at TLM, I offer online classes to empower you the way everyone should be. The education + support I offer gives you experience, evidence, and empathy; you’re getting all of my years of “clinical” RN knowledge, beautifully combined with my real experiences as a mama and a nurse. These are not your average hospital classes (those won’t do it, I promise), and honestly, birth, postpartum, and breastfeeding don’t follow a textbook or protocol anyway. You need to know so much more than that!
If you want to connect with me further, head to Instagram. There are hundreds of thousands of us over there learning together daily.
A note: This post may include affiliate links. This means if you make a purchase after clicking a link, I will earn a small commission (thank you)! Rest assured, this comes at no additional cost to you. You can read TLM’s full disclosure here.
What is postpartum hemorrhage?
First, you should know that it is normal to lose blood volume in both vaginal and cesarean birth. However, a postpartum hemorrhage (PPH) is when there is more blood lost than what is “normal.” Per ACOG, PPH is diagnosed when there is a blood loss >/= to 1000 ml during delivery and additional signs of hypovolemia (low blood volume).
What is normal blood loss after birth?
Average blood loss after birth is about 500ml – 1000ml. Vaginal deliveries are less, about the 500 ml (half a liter) amount. During cesareans (also called c-sections), it’s normal to lose up to 1000 ml (1 liter).
Postpartum hemorrhage is a serious post-birth complication. It is also the leading cause of maternal mortality across the world. When untreated or unresolved, PPH can lead to the removal of the uterus (hysterectomy), shock, or maternal death. Thankfully, PPH is also rare. Overall, it occurs in about 1-5% of births, though it is more likely after a cesarean birth. Typically, a PPH occurs within the first 24 hours after birth, but it can also occur up to 12 weeks after birth.
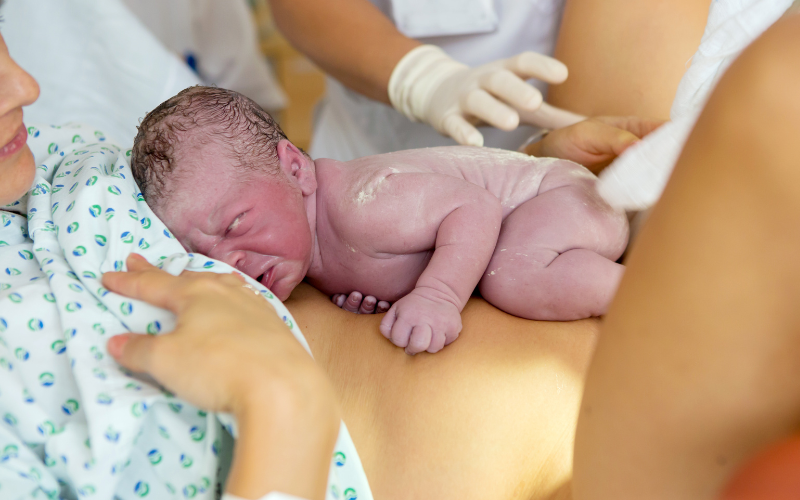
What causes postpartum hemorrhage?
After a baby is born, there are quite a few things happening! First, the placenta delivers in the third stage of labor. After this happens, your uterus should continue to contract. These contractions (called after birth pains) aren’t as strong as labor contractions, but they are important! They help the blood vessels that served the placenta clamp down and stop bleeding. If these vessels can’t or won’t clamp down, there is a uterine tone issue. This means the uterus is soft, “boggy,” and not doing its job! Additionally, some may say it’s being “lazy” or that it is “tired.” When this occurs, those uterine blood vessels bleed freely and a PPH can occur.
In general, there are a lot of possible risk factors for PPH:
- blood pressure issues
- multiples pregnancies (overdistended uterus)
- placental issues (retained placenta, previa condition, acreta condition, abruption)
- medications for labor induction
- multiparity (which means history of prior births)
- obesity
- prolonged labor or rapid labor
- infection
- instrumental deliveries
- existing blood clotting issues
- cervical or vaginal tears
- history of PPH
- Asian or Hispanic ethnicity
- use of general anesthesia
Most common cause of postpartum hemorrhage
Approximately 70% of PPH cases are caused by a uterine tone issue. Many of the conditions or situations on that bulleted list above can lead to uterine tone issues.
What are the 4 T’s of PPH?
The possible reasons for a PPH are easily remembered by “The 4 T’s” Mnemonic. These are overall categories for “why” a PPH occurs. In general, the causes of a PPH will fall into one (or more) of these categories.
- Tone: Tone refers to a uterus that won’t clamp town or maintain tone. Basically, this means it just keeps bleeding.
- Trauma: Trauma bleeding refers to bleeding from tears and lacerations, as well as any uterine bleeding from a rupture or a uterine inversion (when the uterus flips inside out during delivery.
- Tissue: Tissue refers to bleeding from any placental tissues that remain in the uterus.
- Thrombin: Thrombin refers to any blood clotting issues that may be present, like DIC or HELLP syndrome.
Symptoms of postpartum hemorrhage
As mentioned above, PPH is diagnosed when there is a blood loss >/= to 1000 ml during delivery (for vaginal or cesarean birth) and other signs of hypovolemia. Common symptoms of low blood volume may be:
- maternal complaints of dizziness
- headache
- sudden paleness to the skin
- nausea or vomiting
- sweating
- noted increase in heart rate
- drop in blood pressure
- decrease in red blood cell count (Hct)
Typically, a diagnosis of PPH is made after an estimation of blood loss, lab tests (for red blood cell count and clotting factors), pelvic exam, a physical exam, and/or ultrasound.
How is a postpartum hemorrhage treated?
Treatment for a PPH depends on what the believed cause is. The care team may chose to:
- Manually massage the uterus (external fundal massage)
- Give other uterine contractions medications, like Pitocin, Methergine, Hemabate, or Cytotec
- Give additional IV fluids to restore volume
- Perform a pelvic exam and manual extraction of any retained placenta
- Apply oxygen
- Consider devices that block the cervix – these are called tamponade devices (like a Bakri balloon)
- Administer blood products like packed red blood cells or platelets
Most commonly, those who experience a PPH see it resolved at the bedside with some of the interventions on that list. You may need to go to the OR for a D&C (dilation and curettage) if the bleeding cannot be resolved at the bedside. In the OR, your provider can embolize (which basically means block) any uterine arteries that continue to bleed. Lastly, in very, very rare cases, a laparotomy (opening the abdomen to look inside) or a hysterectomy may need to be done.
How to prevent a PPH
Scroll back up to the list of risk factors and causes of PPH and you will see that many of those things cannot be prevented! Explicitly, I want you to hear: “A PPH is not your fault.” You are doing a great job of being here right now, because you are learning about PPH. As a result, you’ll be informed in the rare instance that you experience one.
To prevent PPH, start with considering the care you receive when your placenta is delivering. Both The Association of Women’s Health, Obstetrics, and Neonatal Nurses and the World Health Organization recommend you be given Pitocin during the third stage of labor to help prevent PPH. The Pitocin can be given through an IV or it can be given into a muscle. This is part of something called “active management of the third stage of labor” and it is standard of care in the United States.
If you want to know more about this Pitocin after birth (or are considering denying it), then it is important that you learn about expectant management of the third stage of labor vs active management of the third stage of labor. Then, you can make an informed choice about what is right for you and your body. Also, read up about the Golden Hour and breastfeeding! These are post-birth experiences (hello, oxytocin!) that can help prevent PPH too. All of these topics are fully addressed in my Your Body, Your Birth course!
A comprehensive birth plan can help you clarify your third stage choices, and more! Get mine here.
The takeaway on postpartum hemorrhage
Postpartum hemorrhage is a rare but serious birth complication. It is important to understand its risk factors and the ways that you may be able to help prevent one (so good for you for reading this!). Also, you now know the signs and symptoms of PPH – and that will be helpful for you as you heal and recover at home. Generally, it is best if a PPH is discovered early and treated promptly. If you are ever concerned about your bleeding, don’t hesitate to call your provider and get their help and assessment.
*If you are a student in a TLM course, see the Bonus Lesson: Postpartum Bleeding to help inform you about normal bleeding after birth.
More resources (and freebies!) for you to take a peek at:
- Comprehensive Birth Plan and Birth Priorities templates
- A complete Third Trimester Checklist
- The RN + mama of 4 Ultimate Packing List
- The Labor Mama online birth, baby and breastfeeding classes for every family