If you’re pregnant (or thinking about it), you probably know what an obstetrician-gynecologist (OB-GYN) is. If you aren’t pregnant, I’m going to guess that you may be seeing an OB-GYN right now for your basic preventative women’s health care (menstrual cycle issues, contraception help, pap smears, etc.). I want to put another type of provider on your radar who can do all of that stuff and deliver babies too – a midwife.

Who is The Labor Mama and Why Am I Here?
Hey friend! I’m Lo – also known around here and social media as The Labor Mama. I’ve spent my nursing career in labor, delivery, and postpartum, have birthed 4 of my own babies, have labored thousands of mamas at the bedside, have taught hundreds of students online, and have even delivered a few speedy little babies with my bare hands (oops).
Here at TLM, I offer online classes to empower you the way everyone should be. The education + support I offer gives you experience, evidence, and empathy; you’re getting all of my years of “clinical” RN knowledge, beautifully combined with my real experiences as a mama and a nurse. These are not your average hospital classes (those won’t do it, I promise), and honestly, birth, postpartum, and breastfeeding don’t follow a textbook or protocol anyway. You need to know so much more than that!
If you want to connect with me further, head to Instagram. There are hundreds of thousands of us over there learning together daily.
A note: This post may include affiliate links. This means if you make a purchase after clicking a link, I will earn a small commission (thank you)! Rest assured, this comes at no additional cost to you. You can read TLM’s full disclosure here.
What is a midwife?
Ok, so let’s assume you are pregnant and are wondering what type of provider is best for you and your pregnancy. Maybe you’ve heard of midwives and need more information. Perhaps you don’t love your OB-GYN. Or maybe, your mom is like my mom and asked you “is that safe?” when you mentioned you may see a midwife. Whatever your reason for digging deeper, you definitely need to learn about midwives! So, I’m glad you are here.
Alright, let’s talk numbers for a second. In the US, midwives attend about 10% of births. Despite great outcomes and a holistic, patient-satisfying care model, this number is much lower than other countries. However, I think that as we continue to educate about midwives expertise and skill set, we are going to see that percentage continue to go up.
A midwife is trained to care for you throughout pregnancy and childbirth. Depending on the type of training and licensure, many midwives can also provide standard gynecological and primary health care throughout the lifespan. Midwives may practice at home, in birth centers, in clinics, and/or in hospitals. Where they are able to practice and what they can do is limited by their type of license and credentials. Many of them work alongside OBGYNs. Consequently, they can collaborate with them and, if needed, transfer a higher risk patient to them.
What does a midwife do?
Ok, but what does a midwife actually do? That’s a good question. Here’s a non-comprehensive list of the many things they may do.
- Annual exams
- Pap smears
- Contraception/family planning visits
- Reproductive education (before, during, and after birth)
- Breast exams and care
- Prenatal appointments
- Ultrasounds
- Bloodword
- Routine pregnancy monitoring
- STI screenings
- Screenings/treatment of common vaginal infections and disease
- Attend births
- Basic postpartum newborn care
- Postpartum care and followup
- Surgical assist (with extra training)
Does a midwife actually deliver the baby?
100%, yes! Midwives are trained to handle vaginal birth, from first contraction to placenta delivery and postpartum recovery. They walk next to you throughout your labor, birth, and postpartum care. If you need a cesarean birth, some midwives are trained to be the assisting surgeon (an OB would be the primary surgeon).
Side note: Yes, you can absolutely get an epidural with a midwife! This is a common misconception – and it just is not true. These providers support all types of birth in all types of ways. If you want an epidural and you want a midwife? Great. You can absolutely do that. If you’re interested, here’s a few more common midwifery misconceptions.
What are the types of midwives?
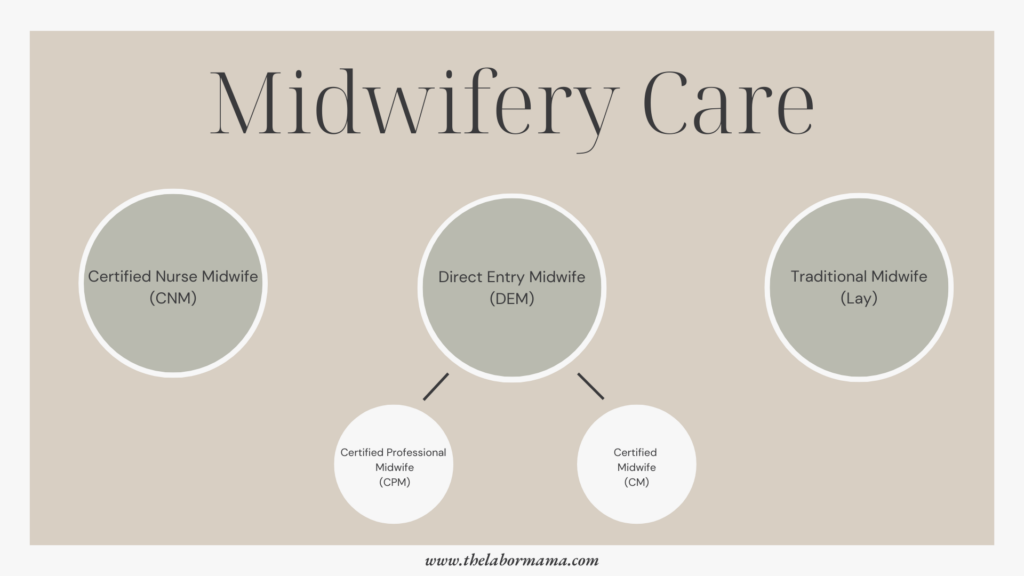
The US is unique in that they have three different types of credentialed midwives. There are also traditional midwives, and it can all get a little confusing. If you decide on midwifery care, it’s important to understand licensure and the types of care the provider can give to you and your baby. You need to understand who you are hiring, what they’ve been trained to do, and what their credentials allow! Let’s go through them one by one.
Certified Nurse Midwives
Certified nurse midwives, or CNMs, are also referred to as advanced practice RNs. Of the different types of midwifery, they have the most health-focused education. Academically, they complete an undergraduate RN program and additional years of schooling for a masters of science in nursing, specializing in midwifery care. Clinically, they have hospital based training as nurses and as midwives. CNMs are board certified by the American Midwifery Certification Board (AMCB) and licensed to practice in all 50 states. Though they usually practice in a hospital, they can provide care at birth centers and homes as well.
Direct Entry Midwives
There are two types of direct entry midwives, certified midwives and certified professional midwives. These midwives can provide care for low risk women in or out of a hospital setting. Unlike a CNM, direct entry midwives are not nurses first. They enter directly into the profession without becoming an RN.
Let me clarify between the two a little bit more.
- Certified Midwives (CM): These providers have a bachelor’s degree in something other than nursing, and then go on to achieve a masters in midwifery. Their training is similar to a CNM and they have the same standards as CNMs, and it is more likely that they chose to work in a hospital and be affiliated with a physician group. CMs are also board certified and they are currently licensed to practice in 13 states. These providers are a newer type of Direct Entry midwife, and we will likely see more of them in the field in the next few years.
- Certified Professional Midwife (CNM): CPMs make up the majority of direct-entry midwives in the US. Typically, these providers are delivering in birth centers and at home, as theirs is the only credential that focuses on delivery specifically for an out-of-hospital setting. Their educational path does not require a nursing degree or a graduate degree and they are certified by the North American Registry of Midwives. Right now, CPMs are licensed and regulated in 31 states.
Lay, Traditional or Community Midwives
The last type of midwife you may know of is a “lay” midwife or a community midwife. There is no certification or licensure for these providers. They believe that they are accountable to care for and serve their communities, and that their care should be free of legislation. Training and learning can be self regulated or apprentice-style, so there may be a bit less similarity across their care practices. Most commonly, these providers perform home births.
Why use a midwife instead of a doctor?
Ok, so why are people choosing midwives? There are certainly some really neat nuances of midwifery care that you may not find with another type of provider. The “Midwives Model of Care” is very different from the care model taught to physicians. Pregnancy and birth are treated as “normal” life events, and care throughout these experiences if often more nurturing, present, hands-on, and holistic. In all of these seasons, technological intervention is minimized as much as possible.
Midwives usually schedule themselves, either alone or with other midwives, in a way that allows them to maximize time with the patient. This usually means that your prenatal appointments may be a little longer and that you will have a midwife at or near the bedside throughout your labor and delivery process.
What are the benefits of using a midwife?
The American College of Nurse Midwives (ACNM) reports a variety of benefits to utilizing midwifery care, including:
- Decreased risk of cesarean
- Less labor induction and augmentation
- Less use of regional anesthesia
- Lower risk of preterm birth
- Lower infant mortality rates
- Less 3rd and 4th degree perineal tears
- Better chance of positive breastfeeding initiation
- Increased satisfaction with care
This is an impressive list, right? Let me throw in one caveat here for those who know and love a great OB-GYN. OBs work with high-risk populations. Midwives typically care for lower risk populations. At times, research results may be skewed toward midwives because the patient population is different. Don’t get me wrong, these benefits are real. But, there are many OBs with excellent outcomes in these areas as well.
Is a midwife right for you?
They really may be! If you are a low risk pregnancy, they are equipped to care for you. And if you are at higher risk, many CNMs work side-by-side with OB-GYNS, and they can still care for you with a doctor’s oversight and collaboration.
I would especially encourage you to consider midwifery care if you are learning towards unmedicated birth or desire more of a ‘wait and see’ approach. Midwives can be an excellent resource for laboring patients with these goals, since they schedule themselves in a way that allows them to be more present at the bedside.
It is important to understand that if you are high-risk from the start of your pregnancy, become high-risk, or need a cesarean delivery, an OB-GYN will become a part of your care or take over your care. If you think a change like this would bother you or cause you anxiety, then a midwife may not be the best choice for you.
The takeaway on midwives
I have worked with wonderful OB-GYNS, FPs, and midwives. Each time I’ve walked on the unit in labor, I’ve truly told my husband that there’s a whole list of people who I’d be more than happy to have deliver my babies – and it includes all types of providers. Ultimately, I don’t think anyone can tell you who to work with – as only you know what types of support best match your hopes and desires for your pregnancy and birth.
* My three pregnancies and births were all cared for by midwives. Here’s my first, second, and third birth stories.

More resources (and freebies!) for you to take a peek at: